Wearable for Health (2017-18)
Introduction
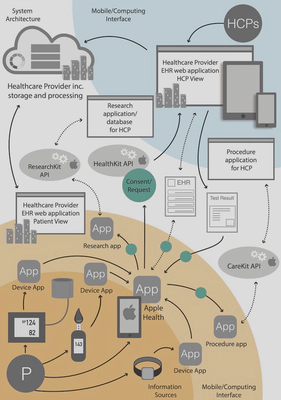
This UX research project explored the use of information from patient-owned smartwatches and smartphones to support patient care prior to surgery. The project also assessed the informational needs of healthcare professionals, asking what data sources they would need from patient-owned smartwatches and smartphones to support care. Through the project research, I identified improvements which were later added to Apple WatchOS and Apple Health for iPhone. These included separating walking and running data, automatically detecting workouts, and providing relational data such as walking distance per day.
Completed Service Blueprint can be viewed at LucidChart.
Client
A healthcare trust, cannot be named due to restrictions related to HRA ethical approval.
Background
While completing an MSc in 2018 I used my dissertation project as an opportunity to explore a real-world area of UX research, wearable devices in digital health. The project focused on healthcare professionals as a user group to ascertain if the information from these devices was fit for purpose prior to creation of apps and software. The research was ethically approved and field work was completed in a clinical setting. The project took place over 6-months.
Objective
To use the problem statement below, as the basis for an in-depth speculative UX research study to be written up as a dissertation and disseminated back to the UX and healthcare communities.
Problem Statement
Could information from patient-owned smartwatches and smartphones be used to support perioperative1 care?
Roles, Methods, and Tools
I was the main researcher. My work was overseen by two supervisors: one supervisor was from a UX/academic background (named principal investigator), and one from a medical practice background, whom I brought on board through my own initiative.
Highlighted methods
Interviews
In preparation for field work, I arranged interviews with professional contacts whom had relevant healthcare experience. I co-created a Service Blueprint diagram with these participants, outlining the patient journey. I also created a glossary, based on the qualitative data from interviews. This was to ensure that descriptive terms used in the recruitment materials, oral presentations, and dissertation were contextually accurate and appropriate.
Alongside this I formed a research collaboration with a healthcare professional working in a relevant role in practice. My collaborator helped to facilitate contextual interviews with healthcare professionals working in a clinical setting. These interviews were used as the basis for discovering data/information requirements. Second interviews were completed with the same participants. I used a lightweight card sorting exercise in the first interviews to allow participants to indicate, which types of health information were pertinent, and the order of importance (from most important to least important).

Survey of Smartwatch owners
I designed a survey, to gauge the attitudes of current smartwatch owners in relation to use of devices for health-related purposes. The survey was distributed via online user communities, social media, and targeted emails. The quantitative findings were presented in the dissertation and used to inform the list and prioritisation of requirements. The open-text responses were used to support human-factors analysis, looking at the likelihood of technology adoption and potential risks.
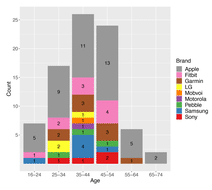
Gallery Image 1 - 75 survey respondents. A key observation is that the 45-54 age group holds the second highest proportion of ownership. These users will be entering the age-based demographics for procedures such as joint replacement over the next 12-20 years. Plotted using RStudio and ggplot2 (Wickham, 2016). Original data is included in Table 1 in the Data section.
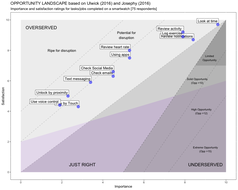
Gallery Image 2 - Opportunity Landscape plot based on Ulwick (2016) and visually inspired by Josephy (2016). All of the smartwatch micro jobs (or small tasks) are in the overserved and 'potential for disruption' part of the plot. This plot shows importance and satisfaction ratings for jobs completed on a smartwatch. 73 – 75 respondents per question. Plotted using an R script custom built by F. MacNeill. Blog post from 2018 featuring more information. Original data is included in Table 1 in the Data section.
Personas and low fidelity prototypes
During the second interviews, user personas based on the scenarios of a hip replacement and a cesarian section were used to consider the viability of the data and information from smartwatches. Low fidelity prototypes of mocked-up data outputs based on the actual data available from a smartwatch, were used with participants to consider how the data could be shown.
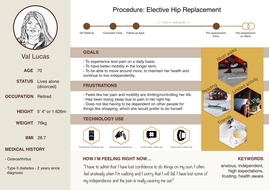
Gallery Image 3 - Persona for Val Lucas, a fictional patient on a care plan for a hip replacement. This persona was based on data from the National Joint Registry (NJR) who track and provide demographics related to joint replacement surgery. Created using Sketch app. Link to PDF for Val Lucas persona.
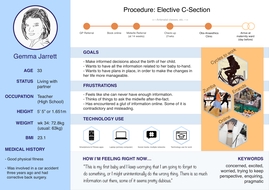
Gallery Image 4 - Persona for Gemma Jarrett, a fictional patient on a care plan for a caesarian section. This persona was based on NHS publications. Created using Sketch app. Link to PDF for Gemma Jarrett persona.
Outcomes
The results pointed to several key areas of opportunity, these were later validated by features and sensors added to the Apple Watch and WatchOS. The project received a mark of distinction.
Answer to Problem Statement
Question: Could information from patient-owned smartwatches and smartphones be used to support perioperative care?
Answer: Yes, with patient informed consent and an appropriate means to deliver information securely to healthcare professionals a patient’s smartwatch and smartphone could be used for this purpose.
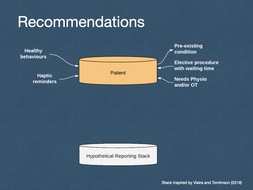
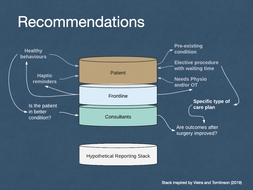
Gallery Images 5, 6, 7 - visualisation of the final recommendations as a reporting stack for software development.
Image 5 - Patient:
- IF the patient meets the criteria:
- [has a pre-existing condition];
- [is having an elective procedure with waiting time];
- [needs physio or occupational therapy(OT)];
- AND would benefit from:
- [adopting healthy behaviours];
- [having haptic reminders].
Image 6 - Frontline staff and Consultants:
- IF the frontline staff and Consultants need to:
- [encourage and monitor healthy behaviours];
- [provide physio or OT - in-person or remotely];
- [are monitoring outcomes after surgery in relation to pre-specified elective care plans].
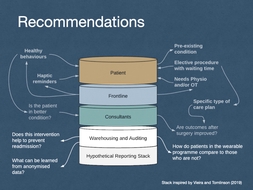
Image 7 - Warehousing and Auditing:
- IF senior managers and auditors need to ask the following questions of the data:
- [does this intervention help to prevent readmission?];
- [how do patients in the wearable device programme compare to those who are not? Are their outcomes better?];
- [what can be learned from the anonymised data?].
Feedback
The clinical practice location where healthcare professionals had been involved in the research invited me back to present my findings. Visual design artefacts including the service design blueprint were included in a juried exhibition at the University of Brighton in 2019 (Show and Tell - The Image in Research). I presented as part of a UX Brighton evening event (12/02/19).
curator of Show and Tell - The Image in Research, exhibition catalogue (2019, p.29).
Reflection
An integral aspect of the project’s success was adopting recognised methods as a framework for the research. I used British Standards Institution’s (BSI) BS EN ISO 9241-210:2010: Ergonomics of human- system interaction. human-centred design for interactive systems. The field of user experience design research was not well known in the clinical context so the standard gave credence to the methods being used.
Had I continued this research I would have validated the Service Blueprint and mental model with a greater number of healthcare professionals working in perioperative care, specifically physiotherapists.
One of the key outstanding issues, as of writing this case study in 2021, is that Apple WatchOS does not allow the user to set rest days/dates. This means that any health-focused app could be undermined by that aspect of the WatchOS. There are however many potential benefits for a seasoned smartwatch user who could ignore or adjust activity reminders alongside a customised app for a patient’s surgical journey.
Data
Table 1
Smartwatch Device Ownership per Age group (data for Gallery Image 1). Smartwatch devices per Age group are listed in alphabetical order.
| Age | Device | Count |
|---|---|---|
| 16-24 | Apple | 5 |
| Fitbit | 1 | |
| Samsung | 1 | |
| 25-34 | Apple | 9 |
| Fitbit | 2 | |
| Garmin | 2 | |
| LG | 2 | |
| Pebble | 1 | |
| Sony | 1 | |
| 35-44 | Apple | 11 |
| Fitbit | 3 | |
| Garmin | 3 | |
| LG | 1 | |
| Mobvoi | 1 | |
| Motorola | 1 | |
| Pebble | 1 | |
| Samsung | 4 | |
| Sony | 1 | |
| 45-54 | Apple | 13 |
| Fitbit | 4 | |
| Garmin | 3 | |
| Pebble | 1 | |
| Samsung | 1 | |
| Sony | 2 | |
| 55-64 | Apple | 5 |
| Garmin | 1 | |
| 65-74 | Apple | 2 |
Table 2
Opportunity Landscape plot based on Ulwick (2016) and visually inspired by Josephy (2016) (data for Gallery Image 2).
Jobs completed on a Smartwatch ordered from highest importance and satisfaction, to lowest.
| Micro Job | Importance | Satisfaction | Opportunity Score |
|---|---|---|---|
| Look at time | 9.6 | 9.7 | 9.5 |
| Review notifications | 8.4 | 8.7 | 8.0 |
| Log exercise | 7.9 | 8.9 | 7.0 |
| Review activity | 7.9 | 9.2 | 6.7 |
| Using apps | 5.3 | 7.5 | 3.2 |
| Check emails | 4.5 | 6.3 | 2.8 |
| Review heart rate | 5.3 | 8.0 | 2.7 |
| Check Social Media | 4.5 | 6.6 | 2.4 |
| Pay by Touch | 2.8 | 4.3 | 1.3 |
| Text messaging | 3.4 | 5.9 | 0.8 |
| Unlock by proximity | 2.3 | 5.0 | -0.3 |
| Unlock voice control | 1.9 | 4.4 | -0.6 |
References
British Standards Institution (BSI) (2010) BS EN ISO 9241-210:2010: Ergonomics of human- system interaction. human-centred design for interactive systems. (Accessed: 2 September 2018).
Josephy, J. (2016) ‘Jobs to be done – a better way to innovate’, Webcredible blog. Available at: (Accessed: 23 March 2018).
Royal College of Anaesthetists (RCoA) (2014) Perioperative medicine the pathway to better surgical care.(Accessed: 31 July 2018).
Stickdorn M. et al. (2018) This is service design doing. 1st edn. Sebastopol, CA, USA: O’Reilly Media.
Ulwick, A.W. (2016) Jobs to be Done: Theory to practice. (Downloaded: 3 March 2017).
Viera, K. and Tomlinson, T. (2019) Blackboard keynote [PowerPoint]. 19th Durham Blackboard Users’ Conference. Unpublished presentation.
Wickham, H. (2016). ggplot2: Elegant graphics for data analysis. 2nd edn. New York, USA: Springer.
Young, I. (2008) Mental models: Aligning design strategy with human behavior. New York, USA: Rosenfeld Media.
-
Perioperative ~ Encompasses the period prior to surgery, during surgery and through to the conclusion of recovery at home; as defined by the Royal College of Anaesthetists (RCoA, 2014, pp. 4-5). ↩︎